A common misdiagnosis
- Ivan Bristow & Jo Rowles
- Sep 14, 2020
- 4 min read
I was recently contacted by a colleague, Jo Rowles in Melton, Suffolk whose patient was suffering from “cracked heels and terrible legs” – not a nice sounding combination so it needed a diagnosis. We discussed the case via e-mail and finally reached a diagnosis. The diagnosis as it turns out, is commonly misdiagnosed as something else and consequently, it is often badly managed so we decided to write this up as a case study jointly, and hopefully, this may help other colleagues to recognize, what is otherwise a common condition.
Case Presentation
The case concerned a 93-year-old woman suffering from cracked heels and “a terrible leg”. Despite her senior years otherwise, she was in good health taking just citalopram 20mgs and occasional paracetamol and zopiclone to help her sleep from time to time. Her medical history revealed a history of leg cellulitis in the past.

She lives at home by herself supported by her daughters and home care. She reported she had had no changes to her health or medication in the last few months. The leg and foot problem had been an issue for about 6 months and had shown little signs of improvement. The patient's main concern was her cracked and scaly heels and swollen leg which felt “tender”. The contralateral leg showed no oedema but distally there was mild erythema and scale extending onto the foot.
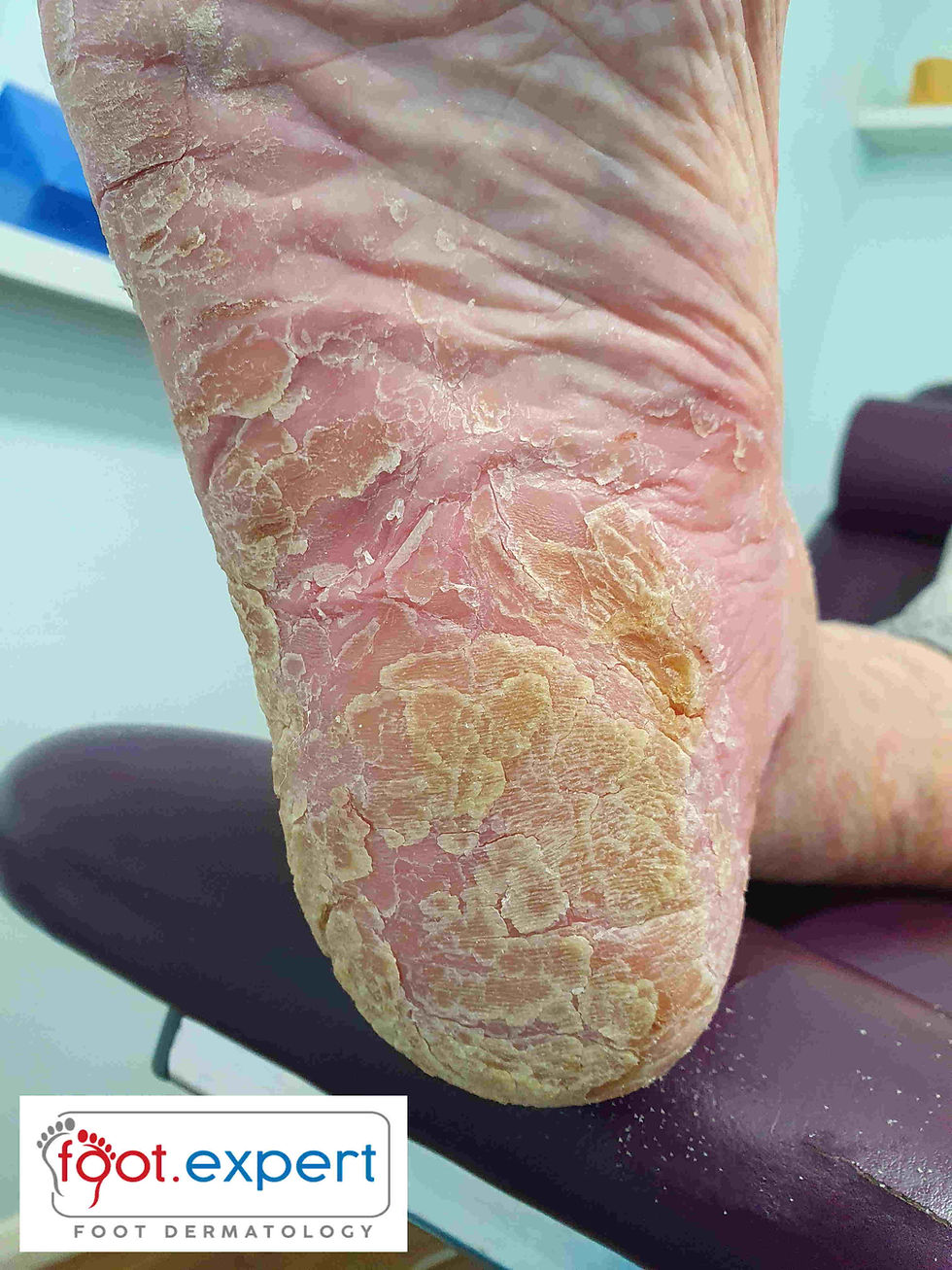
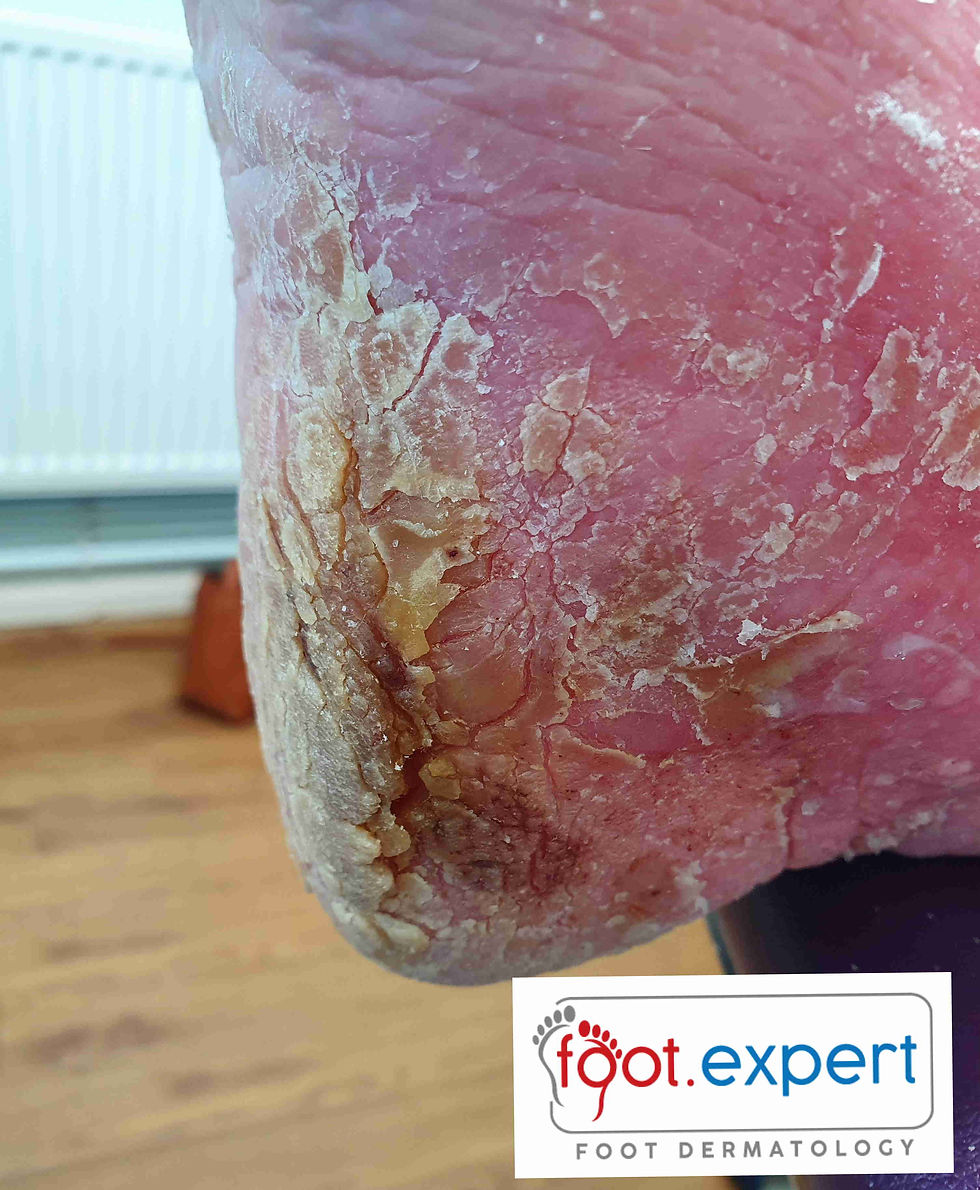
Assessment of the vascular system revealed diphasic pulses and a capillary refill of three seconds. There was no evidence of intermittent claudication or ischaemic related symptoms. Her podiatrist was concerned with the lack of progress and a low likelihood of any dermatology referral, with long waiting times for non-urgent cases.
Discussion
Diagnosis : Venous Eczema (VE)
VE is a common form of eczema that is located on the lower leg and may extend onto the dorsum of the foot and affect the heels. It is most common in the over 70’s age group. Like most conditions, there are known risk factors for its development including:
A history of deep vein thrombosis
A history of cellulitis
Chronic leg oedema
Varicose veins / previous varicose vein or leg surgery
Venous leg ulcers
Obesity
It presents as scaly, crusted areas of skin on the legs that may gradually coalesce to become larger plaques of eczema with an erythemic background. The condition tends to be itchy and may be accompanied by the deposit of haemosiderin in the skin, leaving a permanent brown, rusty discolouration in the gator area. On the foot, the dorsum may exhibit similar features to the leg with scaly, erythema. On the plantar surface, the rearfoot is most often affected and typical features are thick hyperkeratotic areas with fissures that may extend into the dermis. Subsequently, they may ooze fluid or bleed and make walking painful. An impaired skin barrier with scales and cracks leaves the patient susceptible to complications of secondary infection and cellulitis. In addition, the eczema may eventually spread to other areas of the body.
For the patient, it is most likely that the condition developed as a result of previous cellulitis, an inflammatory condition caused by bacterial infection of the skin. The condition, if recurrent can lead to scarring of the lymphatics in the leg, leading to oedema and predisposing to further bouts of eczema and cellulitis. A sudden onset of unilateral leg swelling should always raise the suspicion of deep vein thrombosis and further investigations should be quickly sought.
Misdiagnosis
It is well established that venous eczema is frequently misdiagnosed and treated (incorrectly) as cellulitis (1-4) ending up in potentially unwarranted hospital admission and prolonged courses of antibiotics (5). Both are effectively a clinical diagnosis, but frequent confusion exists on how to discern between the two conditions. The following may help to distinguish:

In addition, in VE patients, particularly with active venous leg ulcers, contact dermatitis is not uncommon and may exacerbate the skin symptoms of VE. Patch testing can be helpful to rule this out if doubt exists (6).
Management
For patients with VE, the aim of management is to improve skin symptoms and prevent further bouts of the condition, or venous ulceration where it is a risk. Typically, this will involve the use of regular emollients, but during the acute stages, the use of topical steroids can be used to bring down skin inflammation in the short term. The use of compression hosiery is also important. Patients should be assessed professionally to ensure that they are suitable for this and to determine the extent of compression required. In patients with peripheral arterial disease, the use of such hosiery may be contraindicated and exacerbate ischaemic symptoms. For the patient, activity should be encouraged such as walking and moving, but standing for long periods of time should be avoided.
Other resources:
Cellulitis – CPD article published in the College of Podiatry journal, Podiatry Now, is available by CLICKING HERE.
References
1. Quartey-Papafio CM. Lesson of the week: Importance of distinguishing between cellulitis and varicose eczema of the leg. BMJ. 1999;318(7199):1672-3.
2. Cox NH. Management of lower leg cellulitis. Clinical Medicine, Journal of the Royal College of Physicians. 2002;2:23-7.
3. Arakaki RY, Strazzula L, Woo E, Kroshinsky D. The impact of dermatology consultation on diagnostic accuracy and antibiotic use among patients with suspected cellulitis seen at outpatient internal medicine offices: A randomized clinical trial. JAMA Dermatology. 2014;150(10):1056-61.
4. Levell NJ, Wingfield CG, Garioch JJ. Severe lower limb cellulitis is best diagnosed by dermatologists and managed with shared care between primary and secondary care. Br J Dermatol. 2011;164(6):1326-8.
5. Weng Q, Raff AB, Cohen JM, et al. Costs and consequences associated with misdiagnosed lower extremity cellulitis. JAMA Dermatology. 2017;153(2):141-6.
6. Tavadia S, Bianchi J, Dawe RS, McEvoy M, Wiggins E, Hamill E, et al. Allergic contact dermatitis in venous leg ulcer patients. Contact Dermatitis. 2003;48(5):261-5.



