Infective Intertrigo - a step on from tinea pedis
- Ivan Bristow

- 4 days ago
- 7 min read
Introduction
The web spaces are an interesting place, dermatologically speaking. Folds of skin, hot, humid often laden with fungus. However, they can also be a source of infection beyond simple tinea pedis. In this blog I will be looking at a not-so-uncommon but potentially severe problem – Infective Intertrigo (figure 1).
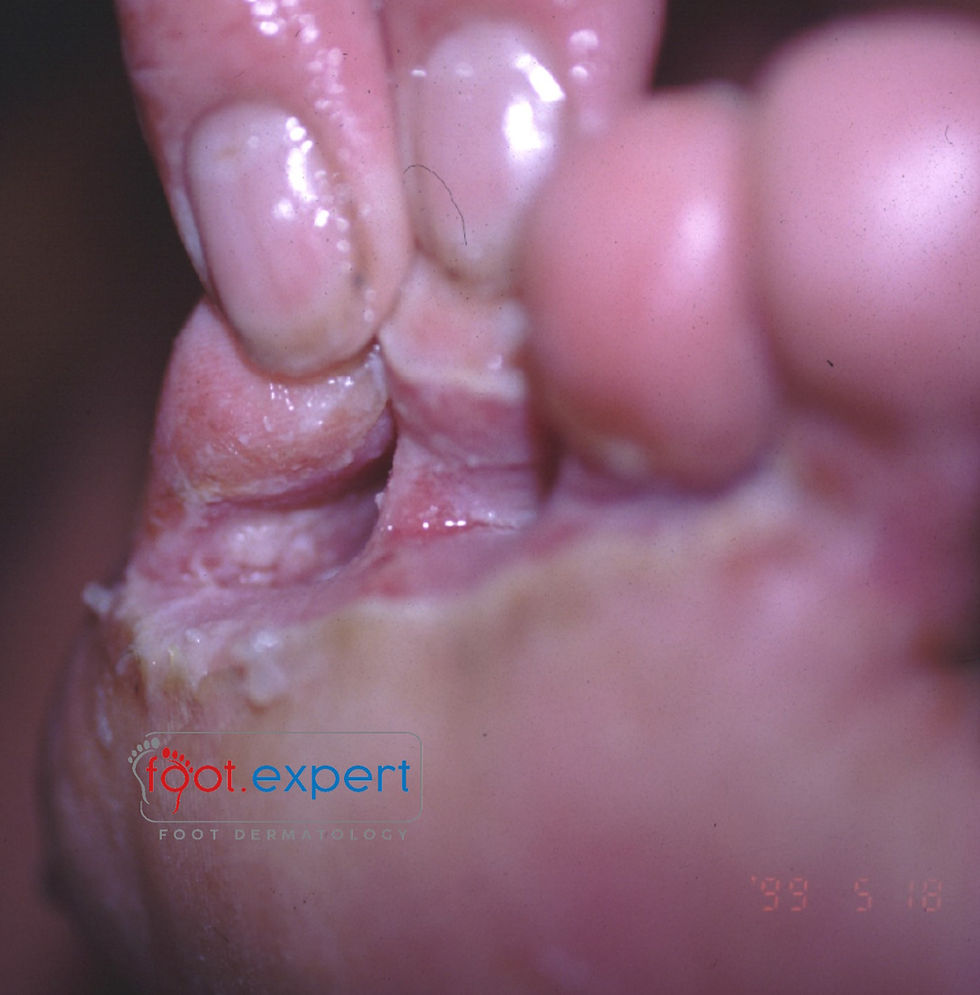
Webspace Infections
Often, we think of interdigital infection as purely fungal affair, but I remember being taught:
“If a web space is dry and scaly think tinea pedis – If its soggy and malodourous consider mixed or bacterial infection.”
Webspace infection goes beyond tinea pedis. The idea of bacterial involvement was first documented by Amonette and Rosenberg in 1973 as a distinct condition [1]. Shortly after, the observations of Leyden and Kligman in 1977 [2] noted that athletes foot had a broad clinical spectrum from mild scale to florid inflammation, itch and skin denudation. However, as they discussed, based on earlier work by Marples [3] and others, the worse the infection was the less likely they were to detect any fungus elements – a paradoxical situation perhaps?

They went on to propose that more severe cases of interdigital tinea pedis were caused by a wider ecological group of microbes involving bacteria interacting with the dermatophytes. Clinically they simplified it into two conditions:
Dermatophytosis simplex: dry and scaly with fungi easily retrieved (figure 2 above).
Dermatophytosis complex: more florid reaction (often with maceration, malodour, hyperkeratosis - figure 1).
Complex infection was characterised by bacterial involvement. Leyden and Kligman demonstrated in a group of 10 subjects with gram-negative bacteria isolated in their webspace, only those with concurrent tinea pedis developed more serious webspace infections suggesting gram-negatives on their own have limited capacity to cause disease but together tinea pedis and gram negative microbes present in the webspace could lead to more serious web space infection [2].
The presence of Bacteria and Fungi in the webspace
The toe webspace naturally a polymicrobic area which contains millions of bacteria which contains both gram-positive and gram-negative organisms, but gram-negatives are only isolated from around 10% of normal toe webs. These include Acinetobacter, Klebsiella, Proteus and Pseudomonas [4]. Studies on toe web infections have identified a range of organisms [5-8] summarised in table 1 below.
Gram Positives | Staphylococci sp. Streptococci sp., Kytococcus sendentarius Corynebacterium minutissimum Corynebacterium xerosis Brevibacterium epidermidis Micrococci
|
Gram Negatives | Pseudomonas sp., Escherichia Coli Proteus Sp. Enterococcus faecalis Serratia marcescens Acinetobacter sp.
|
Fungi | Trichophyton sp., Epidermophyton sp., Candida sp.,
|
In one study, gram negative bacteria could be isolated from around 8% of students, 24% in hospital patients, 41% of industrial workers wearing protective boots [9] and in 58% of miners [9] demonstrating that a damp environment from hyperhidrosis [10] or wet working conditions could promote their growth and development of the infective intertrigo [11].
Clinical Presentation

Although data is sparse, infective intertrigo is documented as a relatively common foot disorder. It presents as erythema, serous or purulent discharge and maceration around the toe webs and occasionally spreading to the adjacent plantar and dorsal surfaces (Figure 3 above). Fissuring, vesicles, oedema and pustules may appear on the surrounding areas.
Denuding of the skin to reveal the red, underlying dermis is a common feature and a hyperkeratotic rim [12, 13] (Figure 3 and 4). Lesions are often malodourous. Unlike tinea pedis which is itchy, patients describe infective intertrigo more often as painful, burning and disabling [14]. The condition has been reported to occur frequently in patients with comorbidities including diabetes, neuropathy and peripheral vascular disease [15].

A key point to remember is web space infection can be due to a broad range of mixed organisms including yeasts and bacteria (Candida, Fusarium, Neoscytalidium, Streptococci, Staphylococcus, Coryneform, Pseudomonas, Proteus and other gram-negative organisms).
Some texts refer to the condition as "Gram Negative Web Space Infection [GNWSI]" however the term "infective intertrigo" has been suggested to more accurately reflect the diversity of causative organisms. Understanding this and the range of pathogens involved is relevant to offer the most effective treatment.
Management
Establishing the diagnosis may be secured with swabs for bacteria and fungal scrapings to guide treatment. Even though the condition has been documented to be common, particularly in specific occupations, there is little consensus on how best to manage webspace infection with papers highlighting non-response to treatment in some cases. The reason for this is unknown but previous research has highlighted that intense fungal/bacterial interaction with the secretion of their own penicillin-like antibiotics could lead to locally resistant bacterial strains [5].
The aims of treatment can be highlighted as:
· Reduction of inflammation and oedema
· Reduction of maceration
· Reduction of fungus/bacteria load
If deeper infection is suspected or the infection is spreading or prolonged with increasing pain, imaging is recommended to rule out osteomyelitis.
Treatment as reported through the literature broadly falls into topical and systemic treatment. Topically, measures should help to address the maceration, infection and inflammation. Managing the damp environment and maceration may be achieved through cleansing, debridement and interdigital wraps or dressings. Agents reported include 2-5% acetic acid, chlorhexidine, povidone iodine, polyhexanide, octenadine and hypochlorous solution may have a cleansing/drying effect whilst offering antimicrobial cover alone or in combination with oral agents when guided by swab results. Where significant inflammation exists the use of topical corticosteroids alongside antimicrobials in the short term can be beneficial. Absorptive Interdigital dressing can help control maceration.
Systemically, antibiotic cover is generally reserved when there is spreading infection, as by definition infective intertrigo is localised, but in some cases, it may progress to cellulitis so antibiosis will be required informed by microbiology results and clinical response to antibiotics. I would recommend that read this 2026 guide for management [16] here for more detailed coverage.
Implications for Podiatrists
The older name of the condition (GNTWSI) can be confusing as noted above, the condition may not purely be gram negative in nature as gram positive organisms may also be present. Consequently, it should be referred to as infective intertrigo for accuracy.
When confronted with a sore or inflamed webspace it is good practice to consider the differential diagnoses - ranging from simple and common to more unusual and problematic:
1. Simple Intertrigo (maceration due to accumulation of moisture in the webspace combined with friction). By its nature it is not an infective condition.
2. Tinea pedis – this can be due to dermatophytes and yeast infections. Typically the web space maybe dry and scaly. Itching may be present.
3. Interdigital psoriasis or eczema. Both conditions rarely, can present with interdigital lesions. These can be difficult to discern visually but a history of lesions elsewhere can help with the diagnosis.
4. Cellulitis. Infection spreading beyond the webspace with increasing inflammation and pain, coupled with systemic markers of inflammation. Usually caused by Staphylococcus aureus.
Malignancy. A rarely reported mimic but two cases have highlight how verrucous carcinoma [17] and melanoma [18] have presented as web space maceration and hyperkeratosis.
In addition, individual cases must be assessed for co-factors such as vascular disease, diabetes and lymphoedema for example. These co-morbidities can hold an increased risk of advancing to more serious, widespread foot and leg infections and may require closer monitoring and follow up.
Finally, research shows that the condition is frequently recurrent with 75% of patients in one study suffering repeated bouts [19]. Often the trigger in these cases, as so often for bacterial invasion, is chronic untreated tinea pedis. Educating patients on basic foot care, spotting the sign of tinea and interdigital infection is key to preventing escalation to bacterial webspace infections.
References
1. Amonette RA, Rosenberg EW: Infection of Toe Webs by Gram-Negative Bacteria. Arch Dermatol 1973, 107:71–73.
2. Leyden JJ, Kligman AM: Interdigital athlete's foot. Postgrad Med 1977, 61:113–116.
3. Marples M, Bailey M: A search for the presense of pathogenic bacteria and fungi in the interdigital spaces of the foot. Br J Dermatol 1957, 69:380–388.
4. Reynolds FH, II, Tusa MG, Banks SL: Toe Web Infections, the Microbiome, and Toe Web Psoriasis: A Review. Advances in Skin & Wound Care 2023, 36.
5. Kates SG, Nordstrom KM, McGinley KJ, Leyden JJ: Microbial ecology of interdigital infections of toe web spaces. Journal American Academy of Dermatology 1990, 22:578–582.
6. Lin JY, Shih YL, Ho HC: Foot bacterial intertrigo mimicking interdigital tinea pedis. Chang Gung Med J 2011, 34:44–49.
7. Yu Q, Li W, Kan S-Y, Liu X-P, Yang H, Gao Z-Q, Chen J, Yang L-J: Clinical Analysis of 57 Patients With Interdigital Infection in Shanghai, China: A Cross-Sectional Study. International Journal of Dermatology and Venereology 2025, 8.
8. Gupta AK, Wang T, Lincoln SA, Bakotic WL: Interdigital and Plantar Foot Infections: A Retrospective Analysis of Molecularly Diagnosed Specimens in the United States and a Literature Review. In Book Interdigital and Plantar Foot Infections: A Retrospective Analysis of Molecularly Diagnosed Specimens in the United States and a Literature Review (Editor ed.^eds.), vol. 13. City; 2025.
9. Noble WC, Hope YM, Midgley G, Moore MK, Patel S, Virani Z, Lison E: Toewebs as a source of gram-negative bacilli. J Hosp Infect 1986, 8:248–256.
10. Aste N, Atzori L, Zucca M, Pau M, Biggio P: Gram-negative bacterial toe web infection: a survey of 123 cases from the district of Cagliari, Italy. J Am Acad Dermatol 2001, 45:537–541.
11. Hope YM, Clayton YM, Hay RJ, Noble WC, Elder‐Smith JG: Foot infection in coal miners: a reassessment. Br J Dermatol 1985, 112:405–413.
12. Fangman W, Burton C: Hyperkeratotic Rim of Gram-Negative Toe Web Infections. Arch Dermatol 2005, 141:658–658.
13. Tan C, Zhang LL, Min ZS: Toe web malodorous maceration with well-demarcated punch-out edge. Int Wound J 2016, 13:1029–1030.
14. Waterton KA, Lipner SR: Gram-Negative Toe Web Infections. Dermatol Pract Concept 2024, 14.
15. Eaglstein NF, Marley WM, Marley NF, Rosenberg EW, Hernandez AD: Gram-negative bacterial toe web infection: successful treatment with a new third generation cephalosporin. J Am Acad Dermatol 1983, 8:225–228.
16. Zeyen C, Abeck D, Becker K, Dissemond J, Kahle B, Lorenzen HP, Löffler B, Maier-Hasselmann A, Mittank-Weidner T, Nast A, Sunderkötter C: S1 Guideline on Infected Interdigital Intertrigo (also called Gram-Negative Toe Web Infection). JDDG: Journal der Deutschen Dermatologischen Gesellschaft 2026, n/a.
17. McKay C, McBride P, Muir J: Plantar verrucous carcinoma masquerading as toe web intertrigo. Australas J Dermatol 2012, 53:e20–e22.
18. Pagliarello C, Paradisi M, Paradisi A: Letter: The most dangerous type of toe web ‘infection’. Int Wound J 2012, 9:108–109.
19. Goiset A, Milpied B, Marti A, Marie J, Leroy-Colavolpe V, Pham-Ledard A, Chosidow O, Beylot-Barry M: Characteristics, Associated Diseases, and Management of Gramnegative Toe-web Infection: A French Experience. Acta Derm Venerol 2019, 99.



