More on Clinisept+
- Ivan Bristow
- Aug 6, 2019
- 5 min read
As promised in my original blog entitled “Goodbye Chlorhexidine?” I wrote that I would follow up that post with further information on a hypochlorous solution (marketed as the product Clinisept+) - a potent antimicrobial agent with significant advantages over the traditional chlorhexidine gluconate used in podiatry for skin preparation (read the original article here).
At the recent Foothealth 2019 meeting in Kettering, there was a lot of interest and I received many questions about it. As the product is relatively new into the market the company, at this stage, are not yet able to give specific indications for its uses. However, in this blog I would like to offer an update and to look at some of the unique properties that make this a useful clinical product for podiatrists starting with common fungal and bacterial infections of the foot.
Fungal Foot Infection
This is a logical place to start as this is the most frequent skin infection we see in practice. Tinea pedis is the most common skin infection encountered in the clinic and for treatment there are currently many suitable products available for topical application to the skin such as clotrimazole, miconazole and terbinafine for example. However, hypochlorous solution may be a new player in this area particularly as it has been shown to have strong activity against fungus and fungal spores, which can be tricky to eliminate.
On that basis, I decided to put the product and its sporicidal action to the test in an area where there is less evidence and where there is a need for a product to destroy fungal elements - in decontaminating socks. For patients with tinea pedis, concomitant fungal infection of their shoes and hosiery frequently exists(1), so there is a need to eliminate fungus from the socks to reduce reinfection rates.
Using an independent UKAS laboratory and applying the EN:20743 standard, I wanted to test the killing power of Clinisept+ against T. rubrum – the common dermatophyte responsible for tinea pedis. Samples sock fabrics were prepared and infected with a T. rubrum culture. Half of the sample were then exposed to hypochlorous solution (Clinisept+), the other half to a control solution of purified water. At the end of the experiment, both the test and control fabrics were measured for viable fungus. The experiment concluded that the Clinisept+ had significant activity killing more than 99.99% of the fungus. The full report of the experiment is now being written up for a journal publication. A second experiment which was run, also showed fast antifungal activity against T. interdigitale - killing greater than 99% of a fungal culture in just 5 minutes.

Figure 1: Clinisept+ can be useful for removing fungal elements from socks soaked overnight in a sealable polythene bag
Clinically, what this suggests is that the product can be useful for decontaminating hosiery from those patients with chronic tinea infection (Figure 1). To this end, I suggest to patients that as part of their antifungal regime. As well as the use of antifungal treatment for their tinea pedis on the skin, that they also treat their socks to reduce and remove any fungal elements using the regime below:
Wash and dry their socks as normal.
Then place them in a sealable polythene bag (such as a freezer bag).
Add the Clinisept+ solution to the bag so the entire socks are damp.
Leave the bag with the socks soaking overnight.
In the morning, remove the socks and wash and dry them as normal ready for wearing.
Of course, it may be easier to for patients to replace their sock collection, but if they are so attached to them this would be a suitable alternative!
Patients I have seen have also tried Clinisept+ as a shoe disinfection spray as well. The product itself should not damage leather as it is water based and doesn’t leave a residue. How best to use it? Well, the product is only active when damp so shoes should be sprayed inside until sufficiently damp and then left to dry naturally. This can be repeated weekly or as needed.
Preventing tinea pedis
In addition, it may have a role in preventing the return of tinea pedis. Some of my patients have taken to spraying, not only their shoes and socks, but their feet everyday. A few minutes of Clinisept left damp on the foot they report as effective at keeping the infection at bay. Another area, for another study perhaps but I am always pleased to have happy patients.
Bacterial Skin Infections of the foot
Superficial bacterial infections of the skin do also arise. Corynebacterium, a gram-positive bacillus, is probably one of the most common superficial bacterial agents observed on the foot responsible for conditions like erythrasma and pitted keratolysis. For the latter, sometimes the use of topical antibiotics such as erythromycin or clindamycin are the only viable option. Antibiotics use, of course, should be minimised so I saw this was another opportunity to test the effects of hypochlorous solution against this particular organism.
In a subsequent laboratory study, I wanted to test its action against Corynebacterium in a manner similar to the T. rubrum experiment. Corynebacterium cultures were exposed to Clinisept+ and a control sample of sterile water for a contact time of 5 minutes and 60 minutes. The results from this lab work showed that exposure of the bacteria to the hypochlorous solution for five minutes destroyed 99.999% of the culture!

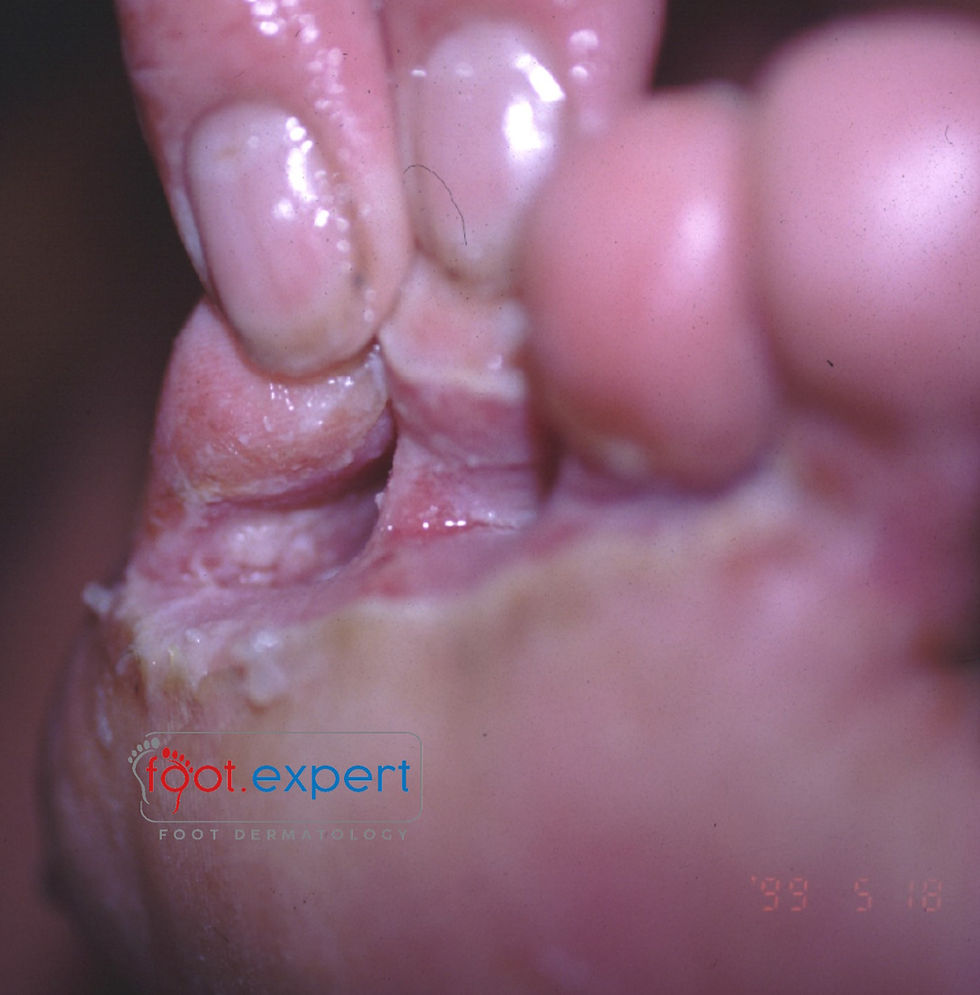
Figure 2: Pitted Keratolysis affecting the 3/4/5 toes and plantar surface
Of course, although this was performed in a laboratory to the EN:13697 standard, would it have any effect clinically? I recently saw a patient with pitted keratolysis affecting his left lateral toes and web spaces (Figure 2, above). I suggested he bathed the area for five minutes, twice a day in Clinisept+, ensuring the area stayed damp during that time to give the maximal effect of the antibacterial properties. He did this by dampening some cotton wool, with Clinisept+ and then placing between the toes and holding it there for a few minutes. The images above and below show the before and after images (Figure 2 & 3), as you can see there is a profound difference with the area now symptom free.

Figure 3: Foot after home Clinisept+ treatment (from patient above)
As a result of this work, I feel confident that hypochlorous solution (Clinisept+) is a great addition to the podiatry clinic and as this work shows, it has great potential as a highly effective, but skin safe, antimicrobial. The product has the added advantage that it can be sold to patients for safe home use for a range of foot problems. In the coming weeks I will be investigating its properties further in the clinic - wound healing. Incidentally, since the writing the first article the manufacturers have announced that they are seeking medical accreditation for specific uses of the product which should enable the product to be indicated for a range of specific applications include fungal infections and wound care - I will keep you updated.
Authors Note:
The author declares he has received no payment from the manufacturer or its distributors in the writing or preparation of this article. The product Clinisept+ is available from a range of Podiatry suppliers and can be used in clinic and sold to patients directly by their podiatrist.
Reference
1. Brown LA, MacLarnon N. Do patients with untreated tinea pedis have concomitant fungal contamination within their footwear and hosiery. Br J Pod. 2007;10(4):134-8.